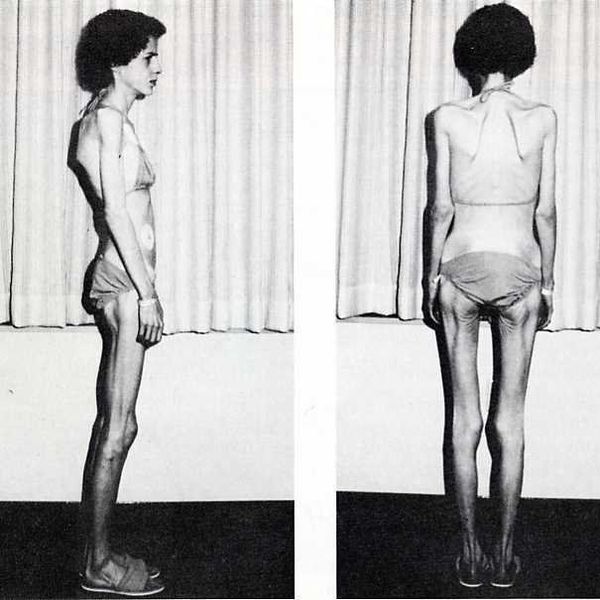
This is an interview I recently conducted with a survivor of an eating disorder. Her name is Karissa. She is a daughter, a sister, a dog mom, and a friend. She's good at sports and comes from a middle-class family. She was Valedictorian of her graduating class. You would never know what she has struggled through just by looking at her. This is her story; this is her testimony.
Trigger warning: I use the term “behaviors” to address any maladaptive behaviors regarding food/exercise. I try to be non-specific as to not trigger those who have yet to find comfort in recovery.
1. When did your disorder begin?
There was not a definitive starting point. The earliest “behaviors” that I can specifically recall occurred in the fourth grade. I would say those maladaptive behaviors ebbed and flowed in severity throughout childhood until I entered treatment.
2. How did it begin?
I remember my soccer coach making generalized comments about the lack of fitness on the team. I was thin and athletic, but did not realize these comments were not directed towards me. If the “big” girls needed to run faster, then why didn’t I? I began to associated thinness with fitness, popularity and worthiness. If I weighed XYZ, I was not worthy of eating specific types and quantities of food.
3. What did your treatment plan look like? How was the journey?
My family and friends had no idea I was suffering. This was my secret, and I believed I was in control of it. Little did I know, that was far from the truth.
At the age of 18 I admitted myself to a psychiatric facility, because I was feeling suicidal and knew, deep down, that I did not want to end my life.
One day, the nurse woke me up to go get morning meds and I fainted in the hallway. This moment was my wake up call. My body was so lacking in vital fluids and nutrients that I could not even stand without my heart struggling to keep up. That moment was when I admitted to myself that my relationship with food/exercise was killing me.
After being medically stabilized, I transferred to an Intensive outpatient program (IOP) out of town. Here, I attended treatment 11 hours a day, 5 days a week. I hated every minute of treatment. I had no privacy; I was escorted to the bathroom and supervised while using sharp utensils in the kitchen. I saw a medical doctor, psychiatrist, and nutritionist weekly. I saw my therapist at least twice a week, in addition to the multiple hours of group therapy a day.
My nutritionist told me what I needed to eat to become “weight restored.” This meal plan was not up for negotiation, you prepared your food and had it approved by dietary staff at mealtime and ate it. However, in the early stages of recovery this was not so simple. My body was not used to consuming enough food and it became physically painful to eat the prescribed amount.
When you were unable to finish your meal you are offered a supplement. The supplement is equivalent to the calories left on your plate, so if you did not finish your veggies you would get XXX calories via an Ensure shake. I approached these shakes as medicine. Once I was healthy, I would never need them again.
I spent a number of months in treatment before returning home. Things were not perfect, and I continued to hide behaviors from my family. I was supposed to continue seeing a nutritionist and an eating disorder specialist when I came home, but I did not. I also failed to stay on my meal plan.
A couple of years later, some major stressors hit my life and I relapsed to the point of needing treatment again. This time, I wanted my life back. I wanted to be able to eat without feeling guilty or questioning myself as to if I ate enough. I wanted to be able to go to the gym because I enjoyed the way my body moved, not to punish myself.
I wanted to be able to throw on any clothing without crying every morning. I wanted to genuinely be able to say, “I do not know what I weigh, and I do not need to know.” This time, my parents were not a motivating factor for recovery, I was. I committed to the program and tried to embrace the concept of mindfulness and self compassion.
When I came back home, I saw a therapist twice a week and regularly saw my psychiatrist every 4 weeks – no matter how stable I thought I was. I followed my meal plan until my therapist and I decided it was safe for me to ease into intuitive eating.
4. Do you consider yourself cured?
No, my recovery will be a lifelong journey. This mindset helps me remember that I am not invincible and that stress can trigger relapse. I have to always be mindful of my thoughts and emotions. Everyday, I choose to be happy.
I chose to see my psychiatrist every month as a preventative measure of sorts. I actively push myself to try things that make me uncomfortable.
5. What is something you would tell your younger self as you were heading down this road?
Honestly, I have no idea. I could list out things that sound nice, but they are not practical.
Truthfully, I think that if I had stronger female role models, I would have reacted differently to some of the pressure I was faced with. That is not to blame anybody for my behaviors, I just may have been a tad less vulnerable if I had some sort of guidance.
6. How is your daily life now?
Amazing. I never imagined I would feel joy again. Sure, I take medication everyday for my anxiety, but so what?
As cliche as it sounds, I enjoy every moment. I am able to exercise whenever I feel like because it makes me feel strong. I honor my cravings and listen to my body. If my body says I need rest, I need to rest (this was a hard lesson to learn).
I’m attending nursing school full time, and hope to specialize in mental health nursing. My boyfriend knows every detail of my past and is supportive of my ongoing recovery; when in doubt, I ask him if he thinks my food is appropriate for my needs. My dog is my secret therapist – she licks me constantly, until I have no choice but to laugh.
7. Is there anything else you'd like to tell the world?
Most eating disorders are not visible to families or even close friends. They occur in silence. Many people remain within a “normal” weight range; this does not negate the fact that restricting, purging, laxative abuse, etc. can cause major damage to your vital organs.
I read an article the other day that said, “If you think you need to be sicker to enter treatment, you are already sick enough.” Your weight does not define you as a person, nor your illness. For me, my eating disorder was a way for me to “control” my 'out of control' emotions. I saw no problem with my behaviors until that day that I fainted.
Eating disorders happen to anybody – regardless of socioeconomic status, family life, and mental health history.