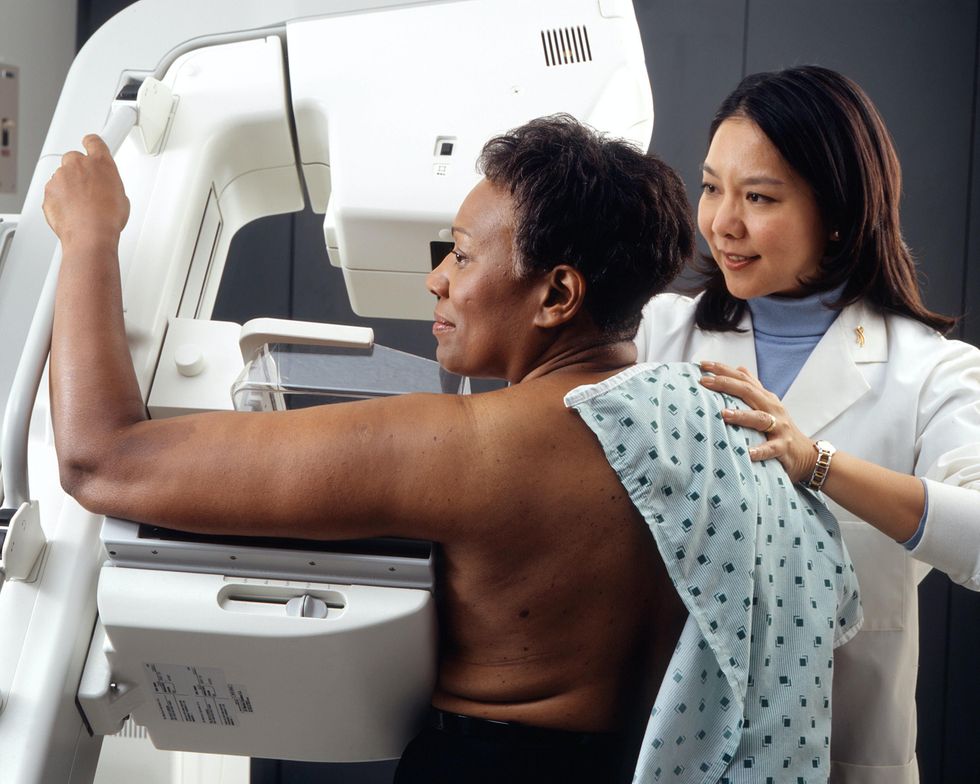
Breast cancer, which claimed the lives of 40,000 women in the United States in 2020, is still a leading cause of death in the U.S., yet there are still a lot of differing opinions surrounding when women should start making mammograms part of their regular healthcare plans. With more than 300,000 diagnoses, however, there is proof that early recognition is a frequent life-saver, and the majority of experts say that 40 is an age when all women should get their first mammogram, and 35 for those women who have family histories of breast cancer.
Breast examinations obviously work, given those numbers, but even so, awareness surrounding the importance of them is still lacking. Women on the younger side of that 40-and-over demographic who should be receiving regular breast cancer screenings tend to be the least informed, and in addition to examining yourself, it's important to encourage your loved ones to do the same.
Baseline Mammogram
A woman's first mammogram is also called a baseline mammogram, and if you're in the 35-40 range you should discuss it with your doctor. For a while, 35 was the proverbial magic number, but most recent studies point to 40 as being a safe bet for the baseline mammogram. After this initial screening, it is recommended that annual mammograms become part of your healthcare regimen.
Though mammograms are recommended as yearly occurrences, other types of examinations can be done periodically without the need for x-rays, and the more often you can perform a detection method, the better, no matter what that method is.
Other Examinations
Before a baseline mammogram, it's good practice to learn how to give yourself a proper breast self-examination, or BSE. Even if you don't plan on conducting a BSE regularly, learning how to perform one will allow you to know what a healthy breast is supposed to feel like in case you ever have any thoughts and decide to conduct a BSE. Clinical examinations are done by trained professionals, and do not require any technology either, and if you happen to go to the hospital for any other reasons, it's a quick addition that could save your life if something is found that requires further exploration.
Some of the sources of further examination for breast cancer include MRIs, ultrasounds, and 3-D mammograms. All three of these processes create some form of imagery that allow doctors and other professionals to analyze the pictures at granular levels. In addition, data surrounding these images can be shared on the grandest scale, allowing for ideas and improvements to be made across the oncology landscape.
With further advancements in imaging and machine learning, these examinations can even provide predictive analysis as to whether a patient may be more or less susceptible to the disease, ultimately allowing them to prepare better for a higher frequency of professional exams if needed.
Awareness
Science is doing its part in lowering the number of breast cancer diagnoses that lead to death, but until the number is zero (or a cure is developed, of course), flattening the curve further depends on awareness both in the types of examinations, and in how important these examinations are.
If you have an opportunity to spread awareness about breast cancer at your workplace, that's a great start, and breast cancer awareness month (October) is almost always a welcomed initiative when asked about in the HR department.
As many businesses appear to be remaining remote, social media is another great place to spread awareness about the disease. There is always a tough line to toe between catching someone's attention and scaring them, but truth be told is breast cancer is a scary thing, especially when untreated. As one out of eight women in the United States will have breast cancer in their lifetime, sharing facts such as that one might be the extra push your loved ones need to start conducting self-exams and ultimately getting their first mammogram.