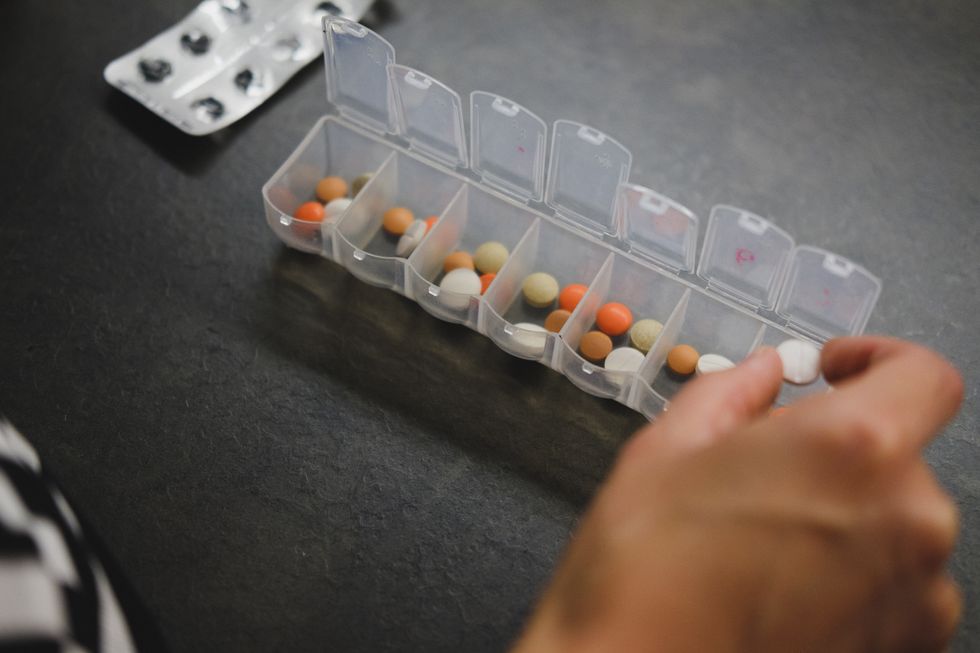
It is a well-known fact that drug prices in America pose near-fatal consequences to the patients who need them. For example, the retail price for insulin is about $300 for one vial. Considering that diabetes is a life-long illness, that is a steep price tag for just staying alive. These high drug costs make America the leading spender per capita for prescription drugs in the world. Throughout the world, however, countries are adopting a financial model that has existed for decades to make drugs more cost-efficient. The model is named QALY: quality-adjusted life year.
The fundamental concept is that the price of a drug will reflect the number of years that the drug provides to the patient after starting the drug. A QALY is basically one year of that person's life adjusted for the hardships that the illness will pose. Each QALY is priced a certain amount, based on health-economics studies into how much Americans want to pay for health care and the country's health-care expenditure relative to the global expenditure.
So, for a healthy 55-year old whose projected life expectancy is 24 more years, this would be 24 QALYs. But for a 55-year old with untreated rheumatoid arthritis, a life expectancy of 24 more years would be muddled with pain and loss of mobility, decreasing quality-of-life and thus would be less than 24 QALYs - let's just assume it is worth 10 QALYs. However, consider that a certain drug would reduce pain and increase mobility - this increases the QALYs to 15. ICER (the Institute for Clinical and Economic Review) has suggested a maximum cost of a QALY to be $150,000. So for this man, one would multiply the additional amount of QALYs the drugs have provided - 5 - by $150,000, which is $750,000 and distribute it over the 24 years. This would mean he pays $31,250 per year.
Now, this seems like a lot of money, but by pushing this concept to multiple pharmaceutical companies, ICER has drastically reduced the retail prices of many important drugs. For example, a cholesterol-lowering drug Praluent, first selling for $14,600, offered to sell it for as little as $4,500. Aimovig, a new migraine drug, expected to cost up to $10,000 a year, went on sale for $6,900. Zolgensma, lifesaving gene therapy for children was priced at $2.1 million when originally its maker said it might cost up to $5 million.
Countries like the UK and Canada have been using this model for years, but American policy has prohibited such an economic concept primarily due to the fact that the country does not want to place a price on life.
So such a moral dilemma comes into play: is it ethically viable to basically place a price on life if the reward is cheaper, life-saving drugs?
The easy debate is that one cannot place a price of life, especially if there is a singular entity determining the cost - that makes that institution practically God. However, many other problems arise especially when you consider who actually suffers these diseases. For example, younger patients would intrinsically have a higher number of QALYs than older patients, forcing them to pay more regardless of how long they actually take the drug. Furthermore, the term "quality of life" is inherently subjective because it is difficult to determine what symptoms are worse than others to create a "worse" quality of life.
Ultimately, however, such a model is proven to drive down drug prices, a troubling issue that affects the lives of many in America. Even though QALYs are understandably highly debatable it is important to consider the reward that they bring.



 Going to the cinema alone is good for your mental health, says science
Going to the cinema alone is good for your mental health, says science











 women in street dancing
Photo by
women in street dancing
Photo by  man and woman standing in front of louver door
Photo by
man and woman standing in front of louver door
Photo by  man in black t-shirt holding coca cola bottle
Photo by
man in black t-shirt holding coca cola bottle
Photo by  red and white coca cola signage
Photo by
red and white coca cola signage
Photo by  man holding luggage photo
Photo by
man holding luggage photo
Photo by  topless boy in blue denim jeans riding red bicycle during daytime
Photo by
topless boy in blue denim jeans riding red bicycle during daytime
Photo by  trust spelled with wooden letter blocks on a table
Photo by
trust spelled with wooden letter blocks on a table
Photo by  Everyone is Welcome signage
Photo by
Everyone is Welcome signage
Photo by  man with cap and background with red and pink wall l
Photo by
man with cap and background with red and pink wall l
Photo by  difficult roads lead to beautiful destinations desk decor
Photo by
difficult roads lead to beautiful destinations desk decor
Photo by  photography of woman pointing her finger near an man
Photo by
photography of woman pointing her finger near an man
Photo by  closeup photography of woman smiling
Photo by
closeup photography of woman smiling
Photo by  a man doing a trick on a skateboard
Photo by
a man doing a trick on a skateboard
Photo by  two men
two men  running man on bridge
Photo by
running man on bridge
Photo by  orange white and black bag
Photo by
orange white and black bag
Photo by  girl sitting on gray rocks
Photo by
girl sitting on gray rocks
Photo by  assorted-color painted wall with painting materials
Photo by
assorted-color painted wall with painting materials
Photo by  three women sitting on brown wooden bench
Photo by
three women sitting on brown wooden bench
Photo by 
 Photo by
Photo by  Photo by
Photo by  Photo by
Photo by  Photo by
Photo by 


 people sitting on chair in front of computer
people sitting on chair in front of computer











